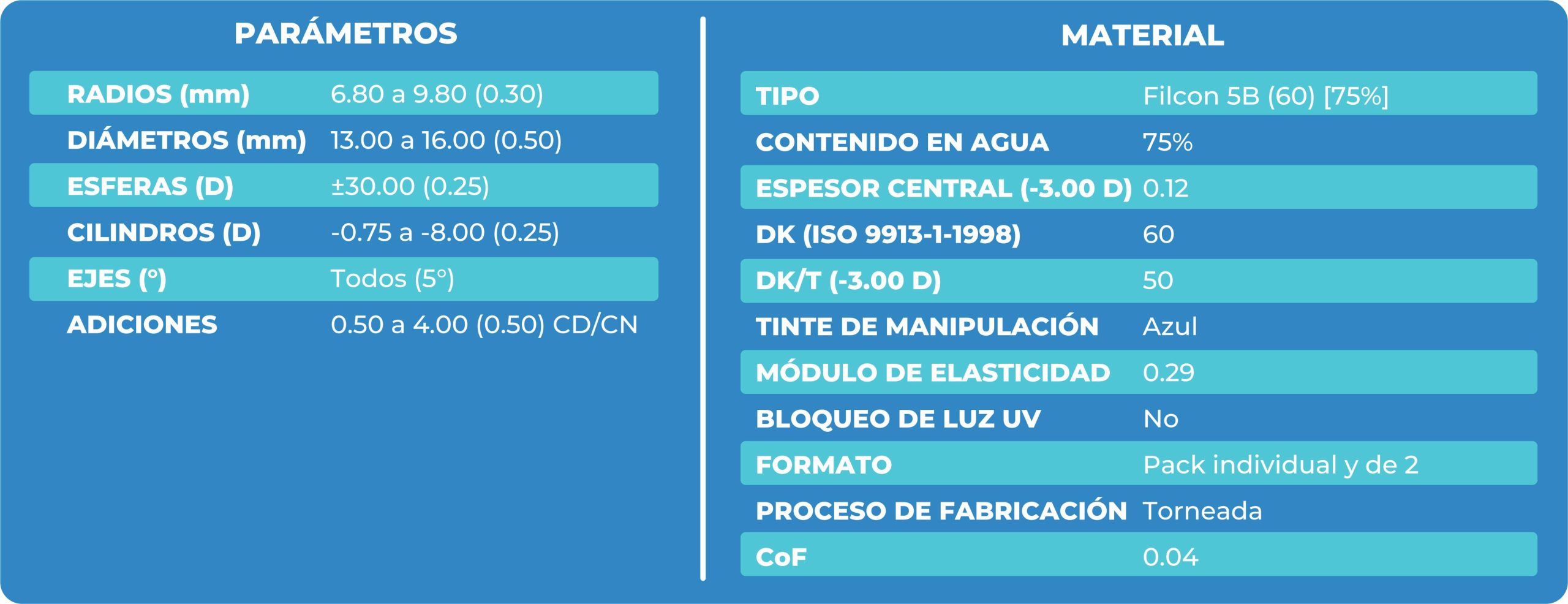
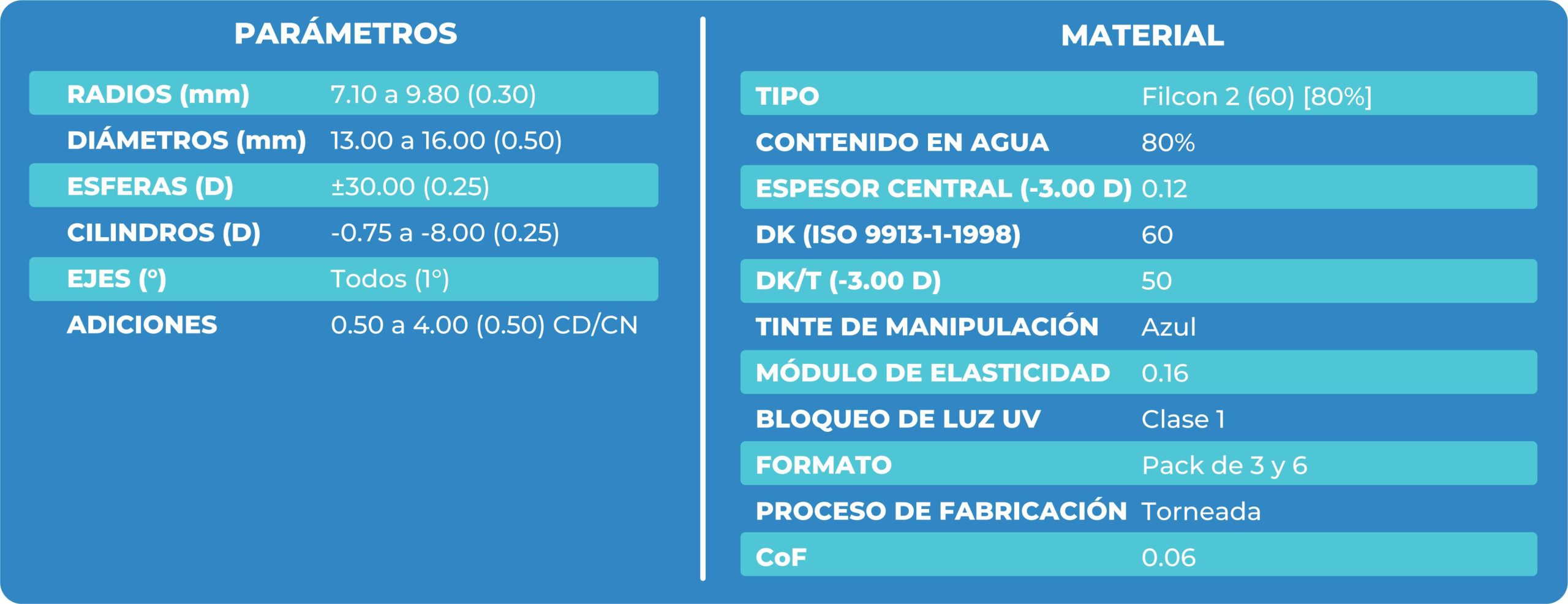
Lens Use

Background
This case reveals a novel presentation of Kc management with the latest and high-end technology contact lens for keratconus management and PKP with high irregularity of the cornea. This corneal irregularity is present with poor vision, which most patients with Kc complain from.
Many patients suffer from small diameter design lenses as foreign body awareness, friction, sometimes lens dislocation and discomfort, which can also induce many mechanical complications like corneal staining.
Case Description
A 51 Year old female complain from unilateral anterior irregularity with PKP.
OD: Kc history with PKP management for the past 12 years,
VA: 0.10
OS: -0.75, managed with glasses
VA: 1.0
The patient was referred to my clinic practice on Jun 15/2022 by Key Ophthalmology Eye Care Center for possible right eye management with contact lenses to improve vision and reduce the headache.
I started over evaluating patient ocular health by objective test with my slit lamp observation and found OD with PKP as a clear and healthy cornea.

Figure 1
During the fitting session to evaluate a scleral lens on a patient who has keratoconus, various amounts of fluorescein can be used between the lens and cornea to understand the proper fitting and fluid amount.
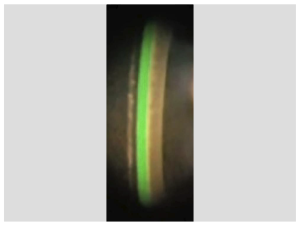
Figure 2
Ideal fitting we achieved after the proper adjustment done.
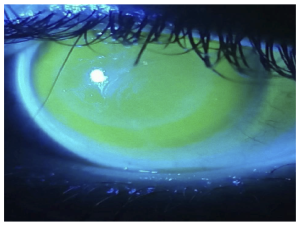
Figure 3
Diffuse light examination using cobalt blue filter to evaluate the general fitting.
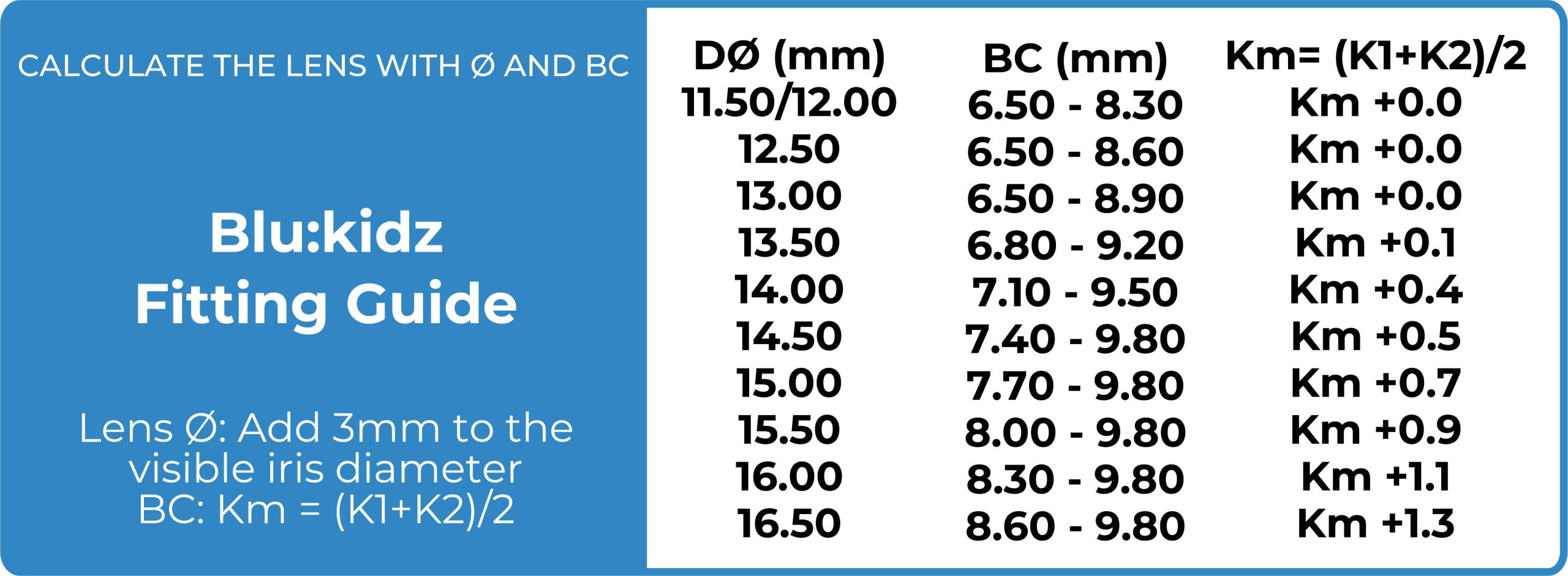
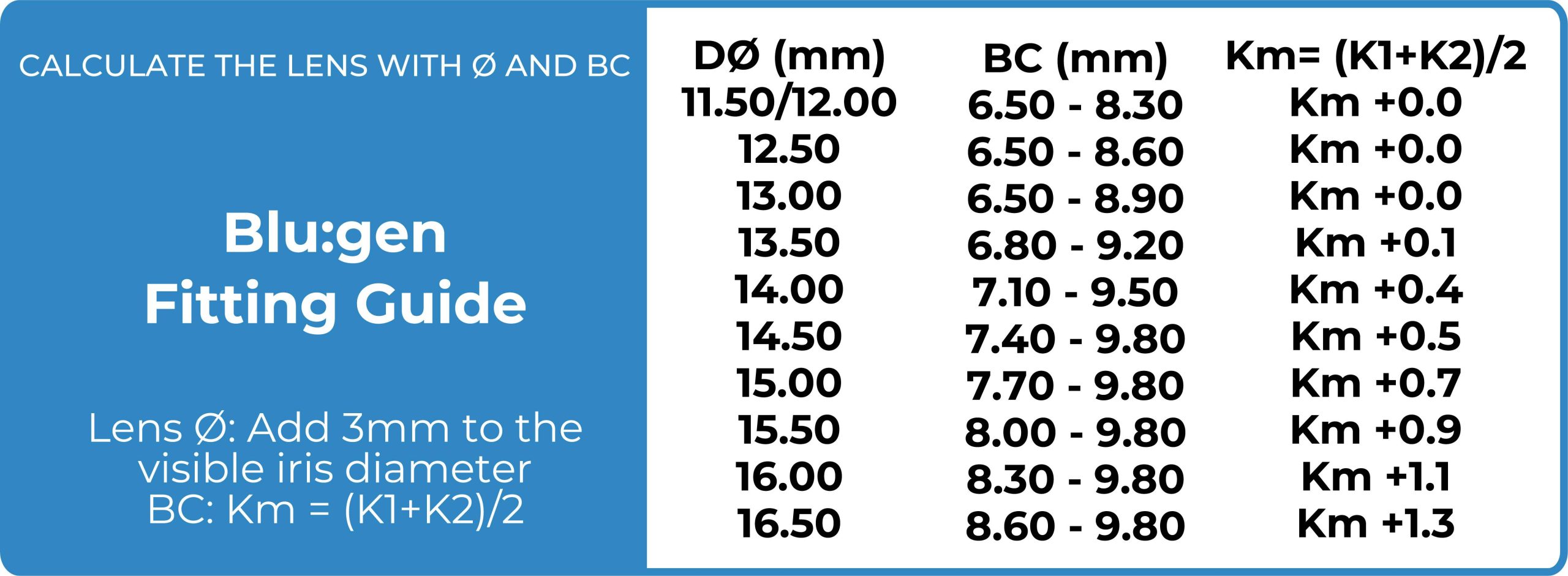
I started with a trial lens with a diameter of 15.5, Sag of 3800, Bc of 8.04, toric edge design, PWR: +2.00 Ds. Initially, the lens was stable and comfortable as the patient expressed and my observations reflected.
During slit lamp evaluation I found the central apical zone was flat with low Sag as 3800 @100 microns after 30 minutes, and I found the mid peripheral settled by 200 microns. The limbal part was appropriate with an average of 75 microns, and the landing part was well aligned horizontally flatter than vertically to meet the scleral shape with no impingements.
Made changes to the lens in the central part by increasing the sag with 150 microns, as shown in figure 2, and I over-refract the case with the lens as the following final Rx: -4.75 Ds.
VA improved up to 0.9
I ordered the final lens with the following: Sag: 3800, BC: 8.04 Dia: 15.50 toric edge design, Total PWR: (-4.75Ds).
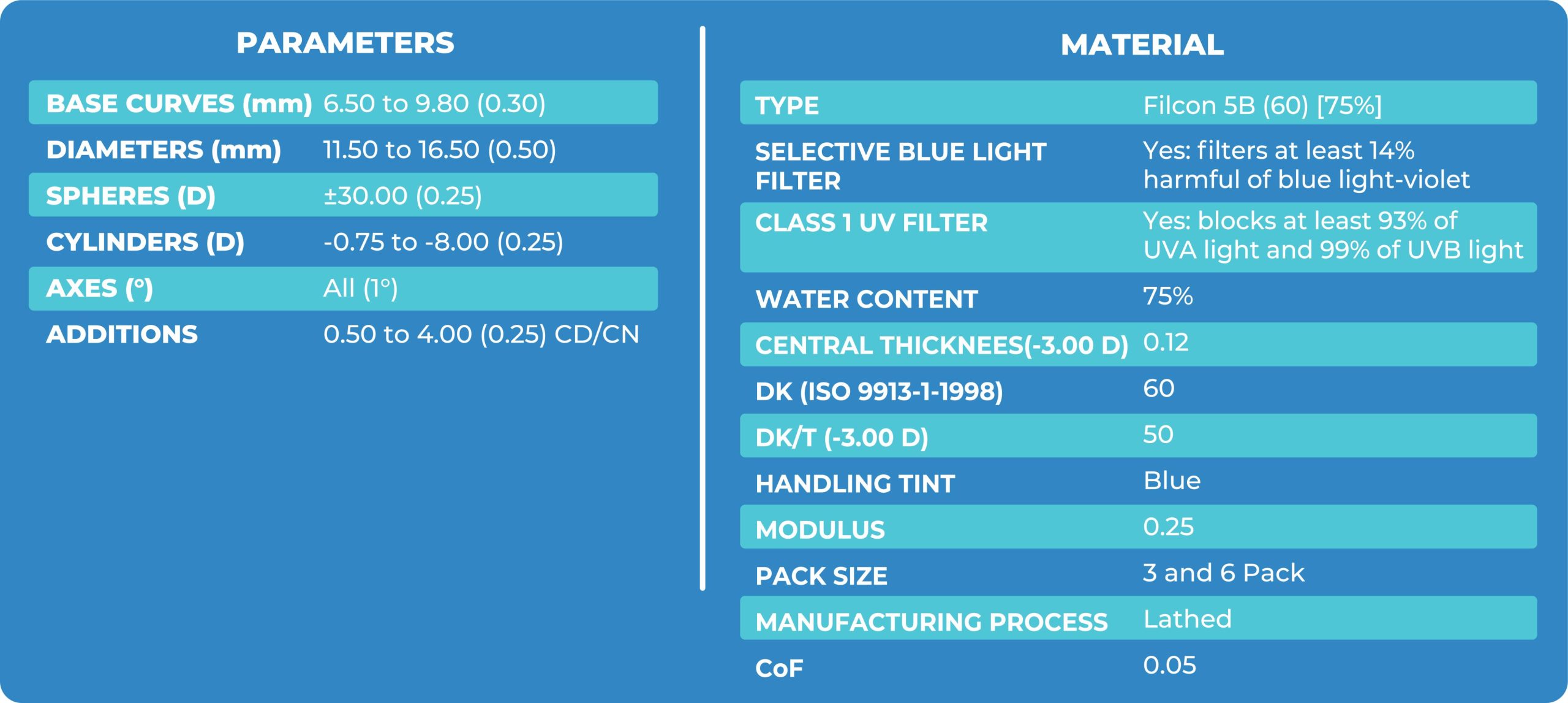
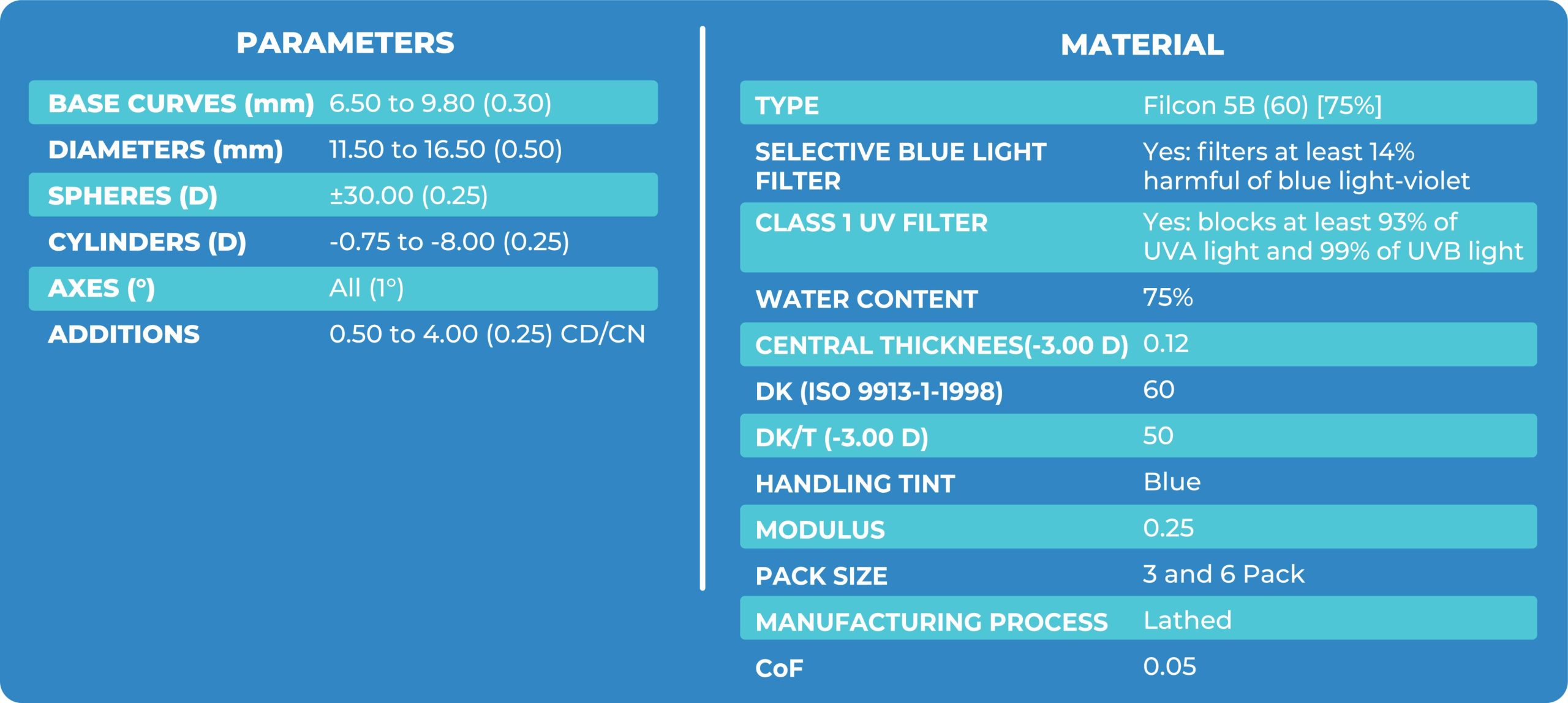
The lens material selected was Optimum extreme to have good oxygen fluxing to the cornea and be away from any expected mechanical complications like hypoxia. I exceeded patient expectations in terms of vision and comfort, which she had lost in the past 12 years.
I received the original lens and we scheduled for the patient an appointment to receive and evaluate the lens required in term of vision, comfort and practice.
All objective and subjective tests were done and satisfied.
“You changed my life” said the Patient."
Conclusion
The case demonstrates how much we can help and improve PKP, Kc, and irregular corneal position with large-diameter scleral lenses made of high-quality materials.
It is vital to ensure that the patient uses the lenses in accordance with eye care professional instructors in terms of hygiene care, insertion solution such as using saline, and so on.
Recommendation

To achieve great performance, eye care professionals should be updated with knowledge and information needed to improve skills and meet patient needs.
They should also prepare the necessary practice units and materials as trial lens sets. I would advise having different trial sets to have different designs to achieve the best fitting consultant and result.
Dr. Nezar Damati
Jordan